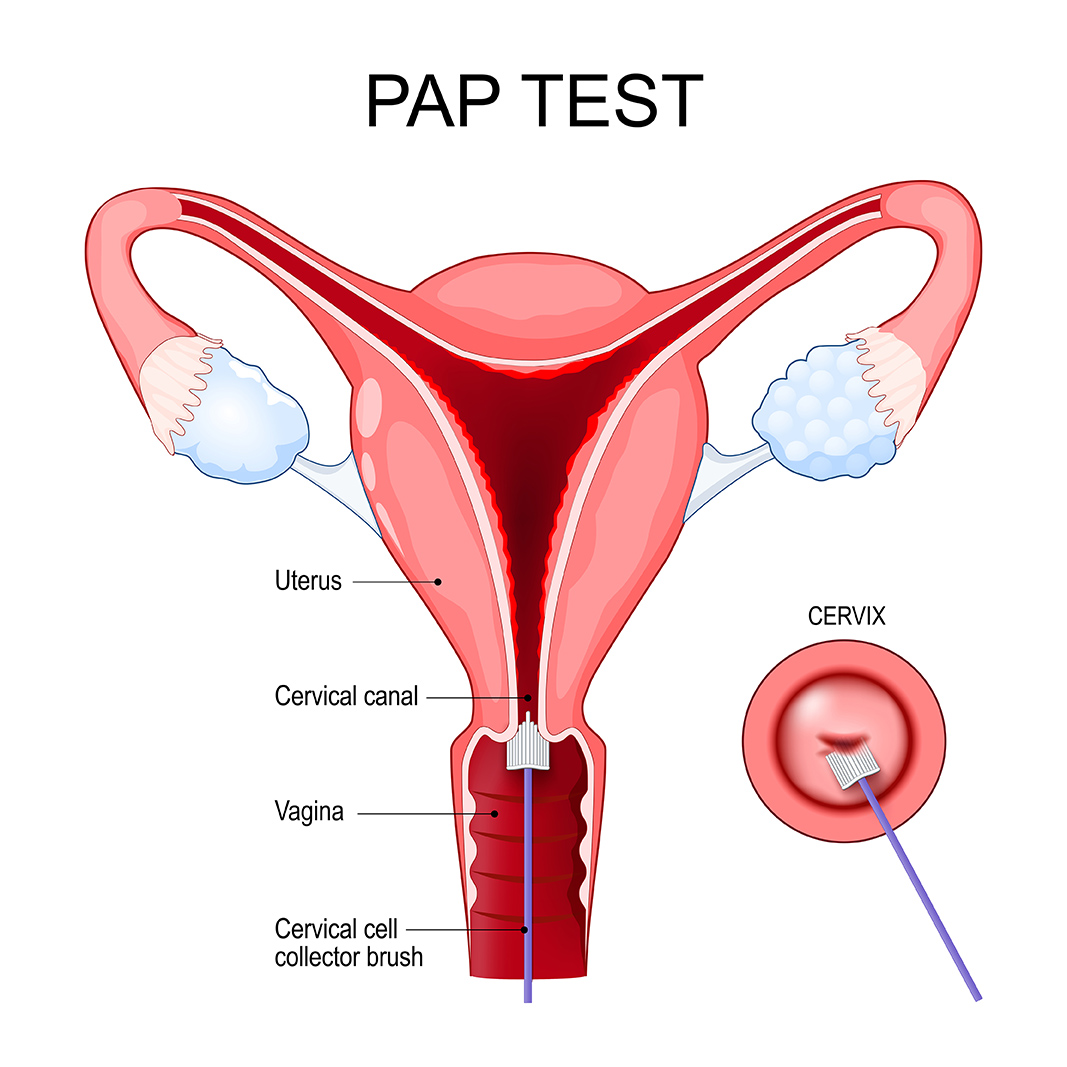
A Pap test, also known as a Pap smear, is a screening procedure that checks for changes in cervical cells. If changes occur over time, it may indicate a problem that requires further investigation. In fact, a Pap test is one of the most effective ways of preventing cervical cancer by catching changes early. However, there are different causes of abnormal Pap tests. Most of these conditions are temporary and can be treated with the proper follow-up care.
Hearing that you’ve had an abnormal test can be scary, but these results aren’t uncommon. It doesn’t automatically mean you have cancer, which is a natural fear when hearing these results read. If you’ve received an abnormal result, there is hope. Most abnormal pap smears are attributed to expected and healthy outcomes that aren’t dangerous.
Explore the reasons for abnormal Pap test results, understand the abnormalities, and learn how follow-up steps can help you continue on your health journey with peace of mind and clarity. The team at Arizona Gynecology Consultants is here to support you every step of the way.
What Is a Pap Test and Why Is It Important?
A Pap test helps detect abnormal cell changes in the cervix. Your gynecologist will gently use a small brush to remove a small sample of cervical cells. These cells are then examined under a microscope to inspect for abnormalities. This screening can help doctors detect early signs of certain conditions, such as precancerous changes, cervical dysplasia, and infections.
Prevention is key, as cervical cancer usually develops slowly over time. Identifying cervical abnormalities early on can help you initiate intervention that will prevent negative changes from progressing. Pap tests are considered one of the most effective tools available in women’s healthcare.
An ideal Pap testing frequency depends on your age, health history, and whether you’ve had abnormal test results in the past.
The Centers for Disease Control and Prevention (CDC, 2025) recommends the following timeline for screenings:
Ages 21-29
The first Pap test should be done around the age of 21.
After this, the CDC recommends repeating the test every three years or sooner if you have concerns.
30-65
Pap tests can be performed every three years. You may also opt for a Pap plus HPV co-test, which can be done every five years.
After 65
If your test results were consistently normal, Pap testing may no longer be necessary.
Since many cervical abnormalities are linked to the human papillomavirus (HPV), combining a Pap test with an HPV test can be beneficial. This is called HPV co-testing and is considered a more accurate screening than a stand-alone Pap test.
Pap tests are more than just a routine appointment or part of your yearly exam. This test can save lives by detecting problems early so you can schedule the necessary treatments to avoid more serious health issues in the future.
What Does “Abnormal” Actually Mean?
Receiving an abnormal Pap test result can be a frightening experience. You may automatically assume that this is a sign of cancer, but that’s not always the case. An abnormal test result simply means that changes have occurred in the cervical cells. This could have been caused by infection, irritation, or a virus, such as HPV. These indications may resolve on their own, while at other times, they may require closer monitoring.
According to the American College of Obstetrics and Gynecology (ACOG, 2025), Pap smear abnormalities can also be more specifically described as:
- Atypical squamous cells of undetermined significance (ASC-US). This is the most common reason for an abnormal test. The designation simply means that the cells look unusual without a clear explanation and are often linked to HPV or mild irritation.
- Low-grade squamous intraepithelial (LSIL). This result indicates a mild change, usually because of an HPV infection. Changes typically correct themselves, especially within younger patients.
- High-grade squamous intraepithelial lesion (HSIL). An HSIL result typically indicates a more significant change in cells that may become precancerous without treatment. Your doctor may recommend follow-up testing after an abnormal Pap test with this result.
- Atypical glandular cells (AGC). Detecting a change in glandular cells may require more detailed testing.
- Atypical squamous cells cannot exclude high-grade squamous intraepithelial lesion (HSC-H). This indicates that abnormal changes are present in the cervical cells, raising concern that an HSIL lesion may be present.
Results can vary widely, from irritation to precancerous changes. Abnormal simply means that your doctor will want to examine you closely to find answers.
Common Causes of Abnormal Pap Results
There are many reasons for an abnormal Pap test result, but most are treatable and temporary. Some examples include:
- HPV Infection – HPV and abnormal Pap results often occur together. High-risk strains can alter cervical cells, but many infections resolve without the need for medical intervention.
- Cervical Dysplasia – This refers to precancerous changes in cervical cells and ranges from mild to severe. Dysplasia may require follow-up visits and additional treatment, but it is very treatable.
- Infections – Various infections can cause abnormal results, such as yeast infections, bacterial vaginosis, and trichomoniasis, which is a sexually transmitted infection that can cause cervical irritation.
- Inflammation or Irritation – Some causes of cervical inflammation can include:
- Sexual activity shortly before your Pap test
- Tampon use
- A recent pelvic exam
- Vaginal douching
- Hormonal Changes – Menopause can lead to low estrogen levels, which can impact cervical cells. Pregnancy hormones can also temporarily alter cervical cells, making them appear abnormal.
- Additional Benign Causes – Noncancerous growths, known as cervical polyps, can appear abnormal under a microscope. Additionally, if you’ve recently undergone surgery, the healing tissue can mimic an abnormal change.
While these causes of abnormal Pap smears can still sound concerning, most of them aren’t cancer or indicators of cancer.
Human Papillomavirus (HPV) and Its Role
Human papillomavirus (HPV) is the most common cause of abnormal Pap results. HPV comprises a group of viruses that are primarily transmitted through sexual contact. In 2024, the Centers for Disease Control and Prevention reported that over 43 million Americans had been infected with HPV (CDC, 2024).
HPV can be separated into two categories:
- Low-Risk Types – These may cause genital warts, but it doesn’t lead to cancer.
- High-Risk Types – These can cause cervical dysplasia. If left untreated, high-risk types may lead to cancer.
HPV causes changes in cervical cells by integrating its DNA with that of the host cells. This can make cells appear abnormal on Pap test results. Most people’s immune systems clear HPV naturally, and the affected cervical cells return to normal.
Because of this, Pap test follow-up steps are very important. If your test shows HPV-related changes, your doctor might recommend another Pap test in a year or a colposcopy after the abnormal Pap to get a better understanding of the cause.
Preventative measures can also help. The HPV vaccine is highly effective at protecting against dangerous strains of the virus alongside regular screenings.
What Happens After an Abnormal Pap Test?
If your Pap comes back abnormal, there’s no need to panic. An abnormal result doesn’t always mean cancer, but rather a result that is different from what’s expected. Your healthcare provider will review the results in more detail and determine the next steps for your care.
Sometimes, minor Pap smear abnormalities are due to infection, irritation, or recent intercourse. If this is the case, your AZGYN provider may suggest repeating the test in a few months to recheck the cells.
Because HPV and abnormal Pap results can be related, your provider may order a test for high-risk HPV strains. This test helps determine whether abnormal cells are linked to HPV, which is the main cause of cervical dysplasia.
If your Pap test results are more concerning, you may need a colposcopy. This in-office procedure involves your doctor using a scope to closely examine the cervix. If the area looks unusual, a small tissue sample may be taken for further study. The biopsy allows your doctor to examine the cervical cells directly under a microscope, confirming whether the changes are mild or significant.
Every woman is different. Your AZGYN provider considers your age, medical history, and test results when determining your follow-up care. It’s important to follow your provider’s instructions. Regular follow-up appointments ensure that problems don’t escalate.
Will I Need Treatment?

Learning you have an abnormal Pap result can be worrisome, but remember – many reasons for abnormal Pap test results don’t require additional treatment. Many changes are mild and tend to resolve on their own, especially in younger women.
Your AZGYN provider may recommend different management options depending on your age, health history, and type of cell changes.
Common options for treatment include:
- Cryotherapy – This treatment involves freezing abnormal cells so healthy tissue can grow back
- Loop Electrosurgical Excision Procedure (LEEP) – The process involves removing abnormal cells with a thin electrical wire
- Close Monitoring – Careful observation with repeated Pat tests and HPV testing can monitor for any changes
When caught early, most reasons for Pap smear abnormalities are highly treatable. That’s what makes screenings so important. Early detection can help prevent cervical cancer later on, giving you the confidence that you’re protecting your long-term health goals.
Preventing Abnormal Results
While not all abnormal Pap results can be prevented, you can take certain steps to reduce your risk of the associated conditions:
- Practice safe sex to reduce your exposure to HPV, the most common cause of abnormal Pap smears. Using protection and limiting the number of sexual partners can also lower your risk.
- Getting the HPV vaccine can be a powerful intervention tool. It protects against strains of HPV that are most likely to cause cervical cancer and precancerous changes.
- Don’t skip annual exams. These visits enable your doctor to monitor your overall reproductive health and note any significant changes.
- Get regular Pap tests in accordance with CDC guidelines for your age and health history.
- Avoid douching or harsh vaginal products that can irritate cervical tissues, disrupt the natural balance of bacteria, and potentially leave you vulnerable to infections.
- Maintain a healthy lifestyle by not smoking and supporting your immune system.
When to Call AZGYN
If you’ve had an abnormal Pap smear and haven’t followed up on the next steps, it’s time to make a call. Even if you’re feeling fine, follow-up testing is essential to understand the reasons behind the abnormal Pap result and its implications for your health.
You should also contact us if you’re experiencing symptoms, such as bleeding between periods, unusual discharge, or pain after intercourse. While these symptoms don’t necessarily mean something is wrong, they deserve attention from an experienced gynecological professional.
Additionally, if you’re due for a regular checkup, an HPV test, or a Pap test, scheduling an appointment with AZGYN can help you take charge of your health. Our caring team can guide you through what to expect, including testing and treatment options, and provide the support you need to care for your health and future.
You’re Not Alone, We’re Here to Help

An abnormal Pap test can feel overwhelming and frightening, but you’re not alone. With the right care and follow-up, most Pap smear abnormalities can be easily managed without much medical intervention.
At AZGYN, we can explain your results, answer any questions you may have, and guide you through the next steps and options. If you’ve had abnormal results or are due for screening, schedule a visit with us today. The team at AZGYN is dedicated to delivering compassionate, expert care, giving you confidence in your health and future.
Schedule a visit with us today. Arizona Gynecology Consultants offers locations throughout Phoenix and the surrounding areas.
Editor’s Note: This article was originally published Jul 9, 2017 and has been updated October 6, 2025.
Sources:
- Centers for Disease Control and Prevention. (2024, January 8). Cervical cancer screening. U.S. Department of Health & Human Services. https://www.cdc.gov/cervical-cancer/screening/index.html
- American College of Obstetricians and Gynecologists. (2023, February). Abnormal cervical cancer screening test results. https://www.acog.org/womens-health/faqs/abnormal-cervical-cancer-screening-test-results
- Centers for Disease Control and Prevention. (2023, October 6). About HPV. U.S. Department of Health & Human Services. https://www.cdc.gov/hpv/about/index.html
The post What Causes Abnormal Pap Tests? appeared first on AZGyn.